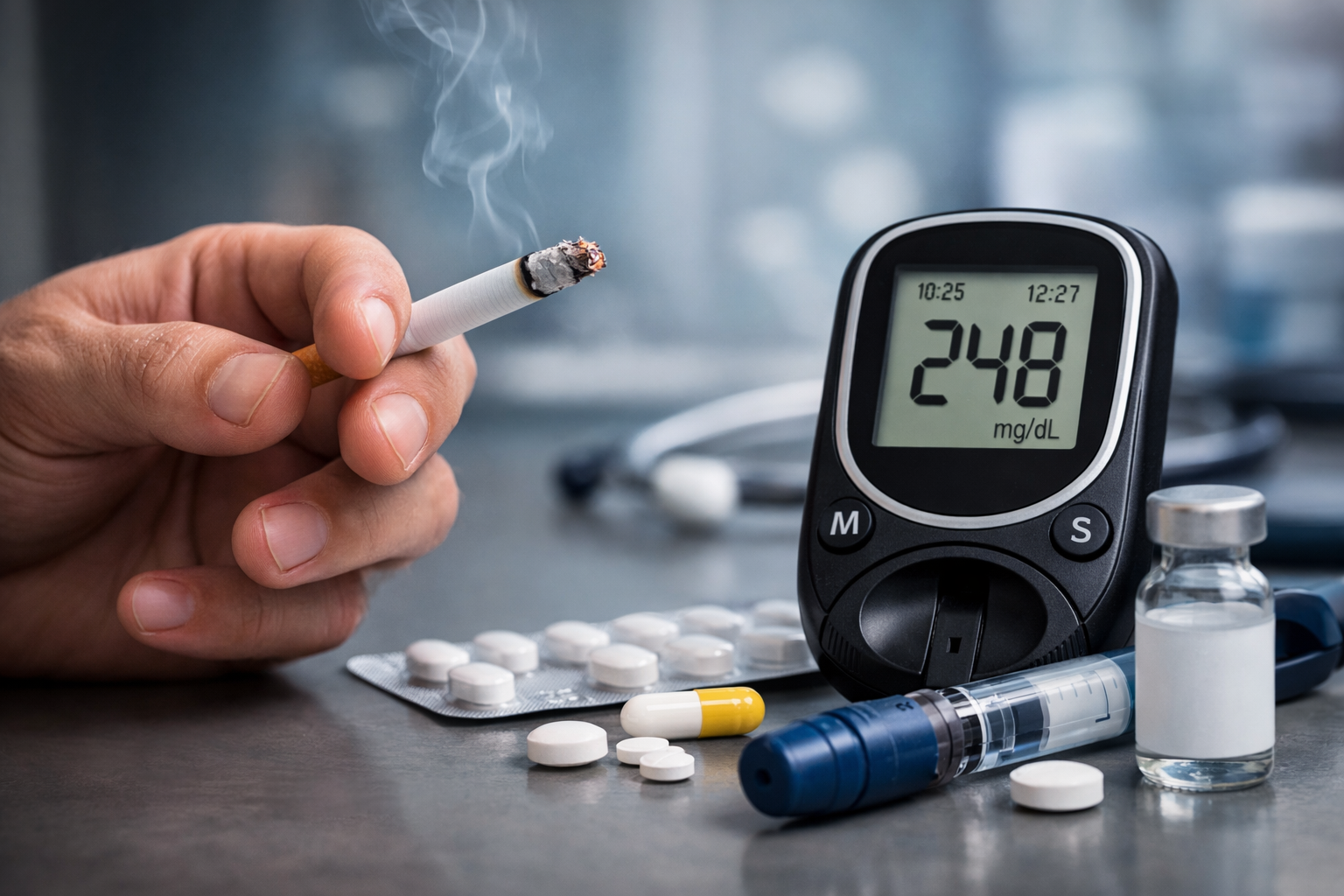
Smoking remains one of the most important — and most neglected — modifiable risk factors in the management of type 2 diabetes (T2D). Despite strong evidence that quitting reduces cardiovascular events, complications, and premature mortality, smoking cessation has yet to be fully integrated into routine diabetes care.
A new CoEHAR commentary published in the Journal of Diabetes highlights what the authors define as “smoking cessation inertia”: a persistent gap between what is known and what is actually implemented in clinical practice.
Globally, around one in five adults with T2D still smokes (20.8%), with even higher prevalence in regions such as East Asia and the Pacific (28.0%) and South Asia (26.0%). These figures are only marginally lower than those observed in the general population, suggesting that a diagnosis of diabetes does not consistently translate into meaningful changes in tobacco use.
This is particularly concerning given that smoking in T2D is not a marginal lifestyle factor, but a major clinical risk amplifier, significantly increasing both all-cause and cardiovascular mortality. In contrast, cessation is associated with improvements in both microvascular and macrovascular outcomes and may also enhance the effectiveness of antidiabetic therapies.
The problem, however, is not a lack of evidence. Rather, it lies in implementation. The commentary identifies barriers at multiple levels:
- at the patient level, factors such as fear of weight gain and diabetes-related distress can reduce motivation to quit;
- at the provider level, time constraints, limited training, and reliance on brief, generic advice often limit effective intervention;
- at the system level, fragmented care pathways, weak follow-up, and limited reimbursement further hinder sustained support.
Together, these factors contribute to a fragmented and under-prioritized approach to tobacco treatment in diabetes care — one in which cessation is rarely operationalized as a core therapeutic outcome.
Addressing this gap will require a more integrated and structured approach, embedding smoking cessation into routine diabetes management and ensuring sustained, personalized support. For individuals who repeatedly fail to quit despite appropriate interventions, the authors also point to a pragmatic role for harm reduction strategies, provided that the ultimate goal remains complete transition away from combustible tobacco.
As the global burden of diabetes continues to grow, the message is clear: the challenge is no longer generating evidence, but ensuring that it is consistently translated into clinical practice.
“We already know that smoking cessation is one of the most effective interventions to improve outcomes in people with diabetes,” said Prof. Riccardo Polosa, co-author of the commentary. “The real issue is that it is still not treated as a core component of care. Bridging this gap means moving from evidence to action — and making tobacco treatment a standard part of diabetes management.”
About the commentary
Adebisi YA, Misra A, Polosa R.
Smoking Cessation Inertia in Diabetes Care.
Journal of Diabetes. 2026;18:e70215.
DOI: 10.1111/1753-0407.70215